24 May The Low Down on Low Back Pain – Part 2
How is lower back pain diagnosed?
Lower back pain is typically diagnosed following a comprehensive subjective and physical assessment by a trained medical professional such as a physiotherapist or a GP. In some cases imaging may be advised to further assess for structural causes of symptoms but these aren’t common cases, and care should be taken in the interpretation of results. I tend to take a very holistic approach in how I tackle assessing and diagnosing lower back pain. Often clients will report a very innocuous movement or position that set off their back pain that they do multiple times a day or week, so I often ask myself the question of “If you’ve done this hundreds of times before with no issues, why did something happen this time?”. This often involves going through a comprehensive subjective assessment of my clients past history, their recent activities, stress and sleep levels, whether anything has changed in their life in terms of their activities to try to find a reason why. Not often do things just happen by chance. Let’s run through some of the common things I discuss with my clients on an initial consultation, it’s important to remember this isn’t an exhaustive list, and my approach will often change depending upon where the client directs the conversation.
Subjective Assessment
History of Symptoms
Determining the history of the current symptoms is often where the discussion will start. More often than not clients will begin with explaining how the episode began – whether that be through a movement or position, or whether it just gradually began from nowhere. This is often one of the most important things to understand as it allows us to dig deeper into the “why” of the symptoms. Next we will often discuss the symptoms that the client is experiencing, this could range from the location of the symptoms, to the severity, the type of pain, how the pain changes with different activities or positions. Developing an understanding of the current symptoms and how they began and interact under different positions and loading patterns is key to understanding the pain and how it affects people.
Past History of Back Pain
In most cases that I see, clients will have a previous history of lower back pain episodes, or they may have an underlying history of persistent lower back pain that may have become aggravated. In cases of clients where they have had a previous history of acute episodes understanding how and when those episodes have occurred is often where I will begin. I will look for a pattern of activities or stressors in the lead up to an episode, or try to determine whether there is a common build up of stiffness or tightness preceding the onset of an episode. This could potentially lead us to developing an ongoing back pain prevention program that clients can put in place both longer term and increase in frequency or intensity if common symptoms were to occur. In clients with a history of persistent back pain it is often more of a discussion surrounding how it presents itself as well as its effect on the clients day to day life. We will also discuss whether they have a management plan in place such as an exercise or mobility program to prevent the risk of acute low back pain episodes.
Current Exercise and Sleep Patterns
The ultimate end goal for all of my clients is to develop an ongoing program that they can complete on a regular basis to reduce their risk of recurrence of pain, low back pain should be treated no differently to any other injury. Determining where the client is currently at with regards to regular exercise routines and sleep routines is key to developing that program. It is very different building an ongoing program for someone who goes to the gym 5xweek for 5 years compared to someone who hasn’t regularly exercises in 3 years. I believe another key is determining what exercise someone enjoys, personally I don’t gain a lot of satisfaction from the gym, I find it a bit slow and tedious, so I perform home strengthening circuits as well as competing in triathlons. If I presented to a physio and they just told me to do a gym program 5xweek forever I probably wouldn’t be too keen to jump on board with that plan. I think physios need to get better at understanding what people want to do as an exercise program – it could be pilates, walking, running, gym, tai chi, yoga or any other number of options. I regular exercise program that someone completes is much better than a program that someone doesn’t enjoy and finds it to be a chore.
Work and Hobbies
As part of understanding our clients as people we should develop an understanding of your work and the life you love to live. Knowing what you do for work day in day out and what you enjoy to do outside of work hours – sport, gardening, playing with your children in the backyard, all form part of the clinical picture of what we are aiming to return you back to. This also allows us to develop an understanding of how your back pain could be impacting your day to day life.
24hr Pattern of Symptoms
The 24hr picture is one of the most important things to understand when looking at a clinical picture. How the pain behaves throughout the day from the minute you wake up to when you go to bed (and even when you are sleeping!) can give us a great deal of insight into potential causes of your symptoms as well as how irritable your symptoms are. Developing a clear picture of how the pain behaves in certain activities such as work – for example sitting could cause an immediate sharp pain in some presentations, but in others could result in a dull ache across the lower back after 3hrs in others, this information can both help inform our diagnosis, treatment plan, and how we manage your symptoms throughout the day.
Nerve Pain/Referral Symptoms
Nerve pain, such as sciatica, can be a relatively common symptom occurring alongside low back pain. Whilst sciatica is the most commonly referred to form of nerve pain there are many differing presentations, some clients may report nerve pain down the outside of their shin, the back of their calf, in their glutes, or down the front of their thigh. Sciatica is simply the presentation of nerve pain along the sciatic nerve pathway. Pain isn’t the only sign of either a nerve irritation or nerve compression, other symptoms could include pins and needles, tingling, numbness, altered sensation, weakness, reflex changes, just as some examples. Referral symptoms are important to map and remember as they are imperative from a diagnostic perspective as well as monitoring treatment response.
Previous Imaging if any
I reckon at least half of my clients who have had a previous history of low back pain (and probably much higher in those with persistent lower back pain) have had previous imaging. Discussing these results along with the symptoms you had at the time and trying to correlate the two are a discussion I will always have. Coupled with that I will try to determine what the clients understanding of the results are and what they mean. More often than not I find clients have been given results and reports but have a limited understanding of the results and what they mean for them – it being written in medical language is often the biggest barrier!
Any Previous Healthcare Providers
Previous history of treatment and who they have seen and what the treatment has involved is a great source of information. Its almost a little bit of a cheat sheet for myself as I can know whether someone has responded well to a particular treatment in the past. Probably the biggest one I will look for is if someone has responded well to dry needling previously, it often isn’t a go to treatment but if someone has responded positively before there is a good chance they will respond positively again. In cases of clients with persistent low back pain it also allows me to understand what hasn’t worked in the past to avoid repeating the same thing. Developing an understanding of whether the treatment plan was passive (lots of hands on and no exercise program) vs active (education, hands on treatment, exercise program) is also key, I often find passive plans may work well short term but have limited long term success and aren’t successful at preventing recurrence. Active programs are, in my opinion, the optimal solution for both short and long term success.
Beliefs about their Back and their Back Pain
Understanding a clients mindset and opinion about their back, the strength of their back, and potential cause of their symptoms is something I discuss with every low back pain client (I actually discuss it with every client regardless of what body area they present with). Negative perceptions surrounding back pain has been found to be correlated with a slower rate of recovery and potential increased risk of developing to persistent symptoms. Unpacking this and discovering the mindset in the first consult is vital. I remember a client of mine who had 7 years of episodic back pain and had been treated by multiple physiotherapists and was told that he was “better”. What hadn’t been unpacked though was this clients underlying fear of his back and potential risk of acute episodes, this fear led to abnormal movement patterns which ultimately increased his risk for future back pain episodes. If this had been addressed as a potential factor earlier in this clients care, improved quality of life, reduced symptoms, and improved time to recovery would all have been potential outcomes for them.
Objective Assessment
Range of Motion
Assessing range of motion is pretty much what every physio will assess for any injury first up. When looking at low back pain we will commonly be looking at range of motion of both the lumbar and thoracic spine, as well as the hip joint. We will often be looking for changes in the way you move as well as symptom production. Often movements to the left and right may feel different to each other if it is one sided pain – determining what each side feels like and the description of the symptoms can be invaluable as a clinician. Assessment of the joints above and below the affected area is routine, it is looking for both overflow effects from the pain, or to assess for any changes that may have predisposed you to the injury occurring in the first place.
Functional Movements and Positions
What even is physio if we don’t take into account function? Day to day life, work, sport, should all be key factors in our examination. In our subjective examination we discussed aggravating movements and positions, now it’s time to test them. One of the more common presentations for lower back pain is pain picking something up from the ground (or potentially higher depending on how irritable it is). We are able to assess your quality of movement as well as symptoms during the movement, this is then able to be retested following treatment to determine improvement.
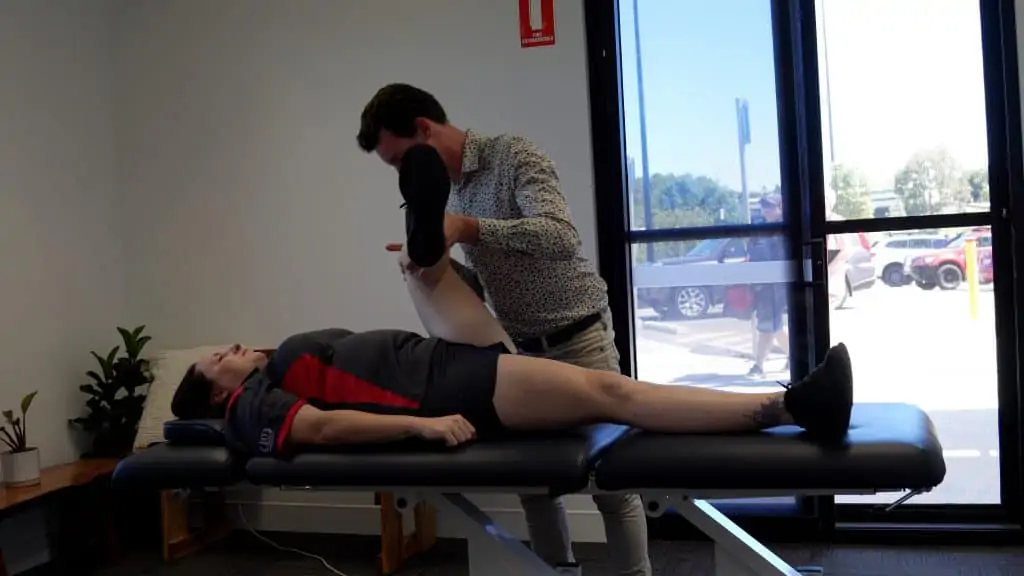
Neurodynamic Tests
These tests are utilised to assess the mobility of the neural system. For the lower limbs and lower back there is three tests, the straight leg raise, slump test, and prone knee bend. All should be utilised in specific situations and to assess for certain diagnoses. The straight leg raise is the most adaptable to assess for different nerves, for example inverting and dorsiflexing the foot would put the peroneal nerve on stretch, if I combine this movement with the straight leg raise and get reproduction of symptoms and can clinically correlate it with your symptoms I am much closer to a diagnosis.
Palpation
Hands on assessments and treatments are unfortunately being utilised less and less in physio these days. I think it should always form part of the assessment and treatment. Understanding what is happening with tissue tone, joint stiffness (though debateable how specific our assessments are), tissue irritability to touch and pressure are all important things to consider as a clinician. If a client has significant muscle tone overlying a stiff joint – if I don’t put my hand son how will I ever know? When assessing using palpation I will often ask my clients how it feels and ask them to let me know if anything is too sore, body language is also a key giveaway to watch for.
Special Tests
Somewhat controversially in physio these days I do use special tests from time to time. These are utilised to rule in or rule out specific structures, in the realm of low back pain the most commonly utilised special tests are those related to the SIJ. There is a significant amount of discussion surrounding these tests and the clinical applicability of them but they can be useful to help fill out the clinical picture if we take their information with a grain of salt and don’t put all our eggs in one basket. The SIJ testing cluster involves a series of tests with the more positive tests you have the greater the chance of the SIJ being the cause of symptoms. They involve torsioning, compressing, distracting, directly palpating the SIJ, and palpating a ligament extending from the SIJ.
How is lower back pain treated?
Lower back pain is best approached from a multi-faceted aspect. The days of mass amounts of hands on treatment, ultrasound and TENS machines, and putting a hot pack on are (or should be) long gone in physiotherapy. We know now that low back pain involves multiple factors ranging from anatomical (joint stiffness, muscle tightness etc), psychological (stress, beliefs, thoughts), and self management strategies (exercise programs, use of heat at home, pain relief), so our interventions need to address all of these factors.
Hands on Treatment
This is a physios bread and butter, we do it better than just about any other profession out there and it’s what sets us apart from most other professions. Hands on techniques can include anything from soft tissue release (massage, trigger point release etc) to joint mobilisations, as well as adjunct treatments such as dry needling. At the end of the day the aim of the treatment is simple, improve mobility and function to allow better adherence to an exercise program and improve quality of life.
Education
In what appears to be a bit controversial in physio these days people are wondering just how much should we be educating – some physios will spend an entire appointment just on education itself. I believe that it definitely forms a major portion of my initial consults but should necessarily come at a cost of hands on treatment, hence why I opted for extended consultations as standard. Ultimately what should be covered in regards to education needs to be entirely client dependant, people will often want to know and understand different things and people understand things in different ways. More often than not most discussions surround a few common topics such as why movement is important, the influence of psychological factors on pain, long term management strategies, and their diagnosis and prognosis.

Self Management
This should arguably be every physios main aim – develop the client into a robust position where they risk of re-injury is lessened, but also to develop an ongoing self management plan should symptoms begin to return where they have a toolbox of strategies to utilise themselves. I believe if clients develop the understanding and skills to manage an episode of back pain, or even better prevent it from getting to that point, I am more than happy with how I have done my job.
Latest Blog Posts
- Lifting Technique “Never Lift with a Bent Back” – Why Those Words Make me Shudder
- When should I see a Physio?
- Adductor Strains – A Footballers Worst Nightmare
- Hamstring Strains – Frustrating, Recurrent, Our process for how we can help you
- Gluteal Tendinopathy – It’s a Real Pain in the Ass
How can we help?
