06 Apr Optimising Exercise Management for ACL Injuries – What you Need to be Doing!
OPTIMISING EXERCISE MANAGEMENT FOR ACL INJURIES – WHAT YOU NEED TO BE DOING!
Having a thorough understanding of the rehabilitation process is imperative. Understanding what it should encompass, what it should look like, and how it should feel for you is all important. In most cases rehabilitation will look similar for each client in the early stages with the aim being to improve mobility and keep muscle activity high. When you reach the middle to later stages, this is the period where it will begin to be differ, a large emphasis is placed on the activities and sport you want to return to. The exercises, dosage and prescription will be tailored to you specifically to have the maximal treatment effect.
Early Management
The early post injury period is an integral time in the management of ACL injuries, it consists of significant swelling and muscle wasting. Minimising muscle strength loss and maximising joint range of motion are both key outcomes. Manual therapy techniques such as massage, joint mobilisations and fascial release techniques to the calf, knee and hip are all necessary. If you are contemplating surgery it is imperative that you return your knee to as close to normal as possible, this means you should have:
- No swelling
- Full knee range of motion
- Less than a 10% deficit in quadriceps strength
This is what is commonly referred to as a “quiet knee”. Clients who do not fit these criteria and undergo surgery will likely be at higher risk of:
- Slower rate of recovery
- Slower return to full knee range of motion – particularly knee extension
- Reduced rate of muscle recovery
- Increased risk of complications or slower healing response
These are among the reasons that lead me to believe that a longer period of rehabilitation prior to surgery is beneficial. It can lead to either not requiring surgery, or if you elect to undergo surgery you will achieve a better outcome.
Exercises in this stage will largely be performed daily or multiple times per day, they can include:
- Stretches
- Isometric exercises – muscle contraction without movement for example a wall squat hold
- Joint range of motion exercises
- Balance exercises
- Single leg loaded exercises if the knee tolerates it
Mid Stage Management
Once the knee has close to full range of motion and there is minimal muscle inhibition, progression towards muscle strengthening will begin. This process will transition towards a gym program as most clients require the capacity to push more than their bodyweight – for example running, jumping or sprinting, or the capacity to absorb high levels of force – for example landing on one leg from a height. From clinical experience, this is the most common area of rehabilitation where clients will not meet their marks. As part of an ACL criteria driven rehabilitation plan PRP Physio has developed, clients should be able to push 1.5 times their body weight on a single rep of single leg leg press. This mark is then expected to progress towards 1.8 to 2 times bodyweight towards the end of the rehabilitation journey. Often, I will see clients who have not been exposed to the necessary load to develop these strength levels, home exercises without weight simply cannot provide an adequate stimulus for this muscle growth.
Change of Direction
Another key component of this time in rehabilitation is the exposure to basic change of direction drills and developing the correct patterns to absorb forces. Implementing basic activities early on can develop confidence in the client’s knee and assist in higher level tasks at later stages of rehabilitation due to the development of the correct movement patterns and technique. This can also lead to a positive psychological effect as clients can often see the progression towards returning to training and being able to have higher participation levels in the sport or activity of their choice. Clients can often struggle to see the end of the tunnel during ACL rehabilitation, as such providing key moments can be the positive motivation they may require. Being able to fast track the return to training is a positive for all involved, it maintains the clients sport specific skill levels, improves coach confidence in the athlete, improves the teams confidence and moral with the athlete as well as improving the confidence of the athlete themselves if training is prescribed appropriately.
Strength and Gym
Once the knee joint has adequately settled following the injury or surgery and the client has normalised muscle activation patterns, you can begin a strengthening program. I strongly recommend that all clients who have sustained an ACL injury obtain a gym membership at this time. The capacity to push a weight that is greater than your total body weight is key in a rehabilitation with an aim to return to sport. In order for a basketball player to jump for a rebound we require pushing our body weight off of the ground from two feet, in order for a soccer goal keeper to run and jump off of one leg they require the capacity to push greater than their body weight off of one leg, there’s are just two of many examples as to why it is imperative we undertake heavy strengthening exercises. Commonly prescribed gym exercises can include:
- Leg extensions
- Squats
- Deadlifts
- Leg press
- Calf raises – both seated and straight legged
- Back extensions
- Step ups
- Hip thrusters
Of course, these are just some of many possibilities that could be prescribed, an appropriate assessment and risk stratification should be undertaken by an experienced health professional prior to beginning a program. Modification of your gym program should be occurring at reassessment intervals with your physiotherapist and this may include changes to; weights, sets and reps, time of reps, for example a slow eccentric with a fast concentric contraction or changing the exercise if pain is present that cannot be altered.
Power
Strength is important, but arguably if considering return to sport, the development of power is just as vital. The ability produce high levels of force quickly is what can be the difference between a player returning to the same level of sport versus a lower level of sport. Like the change of direction skills, basic power development exercises can be introduced in the earlier stages of rehabilitation and progressed as strength develops. Power must be developed in two ways, when considering sport specific demands, players must be able to produce horizontal force (acceleration) as well as vertical force (jump height). Both are equally important, but the weighting will change depending upon the players sport or position they play. Consider a beach volleyball player, they will require high levels of vertical force with less demand for horizontal force, whereas a wing player in soccer will require greater amounts of horizontal force than vertical force due to their greater reliance on speed and acceleration. Coupled with the ability to produce power, a player must also have the ability to absorb the forces following that power development. Consider a basketball player that can jump high, but has poor landing patterns, Derrick Rose may be considered a good example. As an athlete, Derrick Rose had high levels of athleticism and power even in comparison to his peers in the NBA but displayed altered mechanics with his landing patterns which potentially increased his risk profile for sustaining his ACL injury. Whilst I have no insight regarding Derrick Rose’s training programs or injury prevention work, had this potentially been a greater emphasis either prior to or following his ACL injury, his career may have followed a very different path to what it has.
Balance
Throughout all the stages of rehabilitation clients will be performing balance and proprioception exercises, this enhances the body’s ability to know where it is in space as well as improving motor control. Balance is an exercise that needs to be performed in a variety of different ways with increasing mental, environmental and co-ordination demands on the client. If a balance exercise becomes easy and can be held comfortably for 30+ seconds the exercise needs to be progressed. A common progression for soccer players can be the addition of having to pass a soccer ball whilst balancing on one leg, this could then be progressed to performing the same activity on an unstable surface. An example of increasing mental demands could be balancing on one leg with your eyes closed counting down from 100 in 7’s. Clearly there is a huge variety of exercises that can be performed to improve balance and proprioception, it is about keeping an exercise challenging to force the balance system to recognise it needs to perform better whilst challenging different elements and environments.
Typical Rehabilitation Timeline Guided by Months
This is a guide only and is not indicative of how every client’s rehabilitation will progress, the process is a journey and as such there are ups and downs along the journey. Some clients may progress faster, and some may progress slower, the end goal and demands you will place on the knee will also dictate how fast or slow it is recommended you progress.
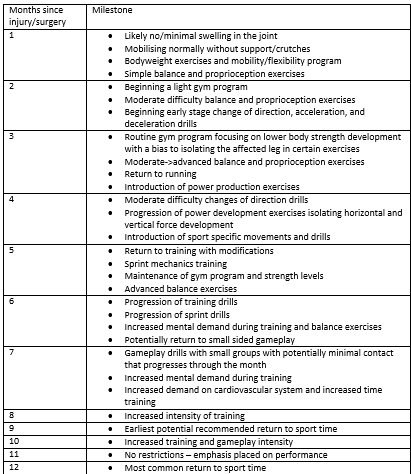
This timeline can often be difficult to predict for some clients, some will experience a smooth journey with minimal issues whilst others may have complications arise which will set back their recovery. As such this should be taken as a guide only, non-surgical recovery process will look slightly different, it will most commonly be the same journey but compressed into potentially a 6 month or less timeframe. The reason for this change in timeline is that post-surgical clients require time to recover from the surgery as well as allow time for the ACL graft to mature and increase in its strength. The process it undergoes is that the graft will reduce in strength over the first 6-12 weeks and then will gradually increase again. Research has been unable to conclusively identify at what timepoint the ACL graft is considered “mature” with ranges from months to years.
Sport Specific Drills
Whilst returning to sport for some clients can often be enough, returning to the same level of sport and performance level is essential for many. Accurate exercise prescription and progression of field-based drills to an adequate intensity is a necessary skill for any practitioner working in this environment. Field/court-based drills including change of direction, agility, jumping, landing, contact and skill-based work must all be prescribed. Initially all of these will be prescribed separately, as the client progresses the tasks will become more complex with the addition of multiple factors. For example, a basketball player may start with a rebounding drill focusing on the jump and landing aspect. As the player progresses, this drill could include a second person to compete for the ball, or they could have to land and then turn to pass or run, or could be the addition of a quick second jump to further emphasise power production. Through my experience, this is a common area that can be missed or underdeveloped in a lot of clients looking to return to sport. I believe both a lack of facilities in most clinical environments as well as preconceived therapist beliefs (the belief that we have to perform hands on treatment) are large barriers to this and is something physiotherapists as a profession should move past for the benefit of our clients.
